Yakima
(509) 225-3668
Ellensburg
(509) 925-4633
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.

Athlete's foot is a common fungal infection affecting the skin on the feet, particularly between the toes. Symptoms include itching, burning, and stinging sensations, often accompanied by redness, peeling, and cracking skin. The affected areas may also appear swollen and develop blisters. Diagnosis typically involves a physical examination by a podiatrist, who may scrape a small sample of the affected skin to examine under a microscope or send it to a lab for testing. Identifying the presence of fungal elements confirms the diagnosis. Early recognition and treatment of athlete's foot are essential to relieve discomfort and prevent the infection from spreading. Proper hygiene, antifungal medications, and keeping the feet dry and clean are effective measures to manage and prevent athlete's foot. Athlete’s foot can be uncomfortable and unsightly. If you have any of the above symptoms, it is suggested that you consult a podiatrist who can successfully treat this condition, which may include prescribed medication.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with one of our podiatrists from Cascade Foot & Ankle. Our doctors will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.
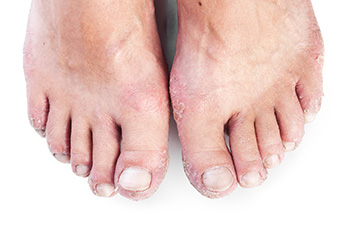 Psoriasis of the feet, particularly palmoplantar psoriasis is a chronic skin condition characterized by thickened, red, and scaly patches on the soles. This form is often accompanied by painful fissures and can severely impact mobility. Another variant, localized pustular psoriasis, presents as pus-filled blisters surrounded by inflamed skin. Nail involvement is common, leading to pitting, discoloration, and onycholysis, or separation of the nail from the nail bed. Triggers for psoriasis include stress, infections, skin injuries, and certain medications. Diagnosis is primarily clinical, supported by a skin biopsy if necessary. Treatments range from topical therapies like corticosteroids and vitamin D analogs to systemic treatments, including biologics and oral medications for more severe cases. Phototherapy is another effective option. In refractory cases, surgical intervention may be considered to remove painful, thickened plaques. If you have discomfort in the feet from psoriasis, it is suggested that you schedule an appointment with a podiatrist for optimal management and personalized care.
Psoriasis of the feet, particularly palmoplantar psoriasis is a chronic skin condition characterized by thickened, red, and scaly patches on the soles. This form is often accompanied by painful fissures and can severely impact mobility. Another variant, localized pustular psoriasis, presents as pus-filled blisters surrounded by inflamed skin. Nail involvement is common, leading to pitting, discoloration, and onycholysis, or separation of the nail from the nail bed. Triggers for psoriasis include stress, infections, skin injuries, and certain medications. Diagnosis is primarily clinical, supported by a skin biopsy if necessary. Treatments range from topical therapies like corticosteroids and vitamin D analogs to systemic treatments, including biologics and oral medications for more severe cases. Phototherapy is another effective option. In refractory cases, surgical intervention may be considered to remove painful, thickened plaques. If you have discomfort in the feet from psoriasis, it is suggested that you schedule an appointment with a podiatrist for optimal management and personalized care.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact one of our podiatrists from Cascade Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions, please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.

A bunion, medically termed hallux valgus, is a bony protrusion on the inner side of the foot, precisely at the base of the big toe. This condition arises from the misalignment of the bones in the forefoot, compelling the big toe to angle towards the lesser toes, consequently protruding the joint at its base. Bunions can cause significant discomfort and interfere with your daily activities. If you have exhausted nonsurgical options like padding or orthotic shoes, bunion surgery may be the next step to relieve your pain and improve mobility. During the procedure, a podiatrist may remove the bunion, realign bones, or release tight ligaments to straighten your big toe. Risks of bunion surgery include nerve damage, bone healing issues, or overcorrection. The recovery process often takes up to six months. Initially, you may need to keep your leg elevated to reduce swelling, and it can take weeks before you can comfortably wear regular shoes again. Among the long-term benefits of bunion surgery are improved comfort and mobility. If you are struggling with bunion pain, it is suggested that you consult a podiatrist to discuss whether surgery is right for you.
If you are suffering from bunion pain, contact one of our podiatrists of Cascade Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
In most cases, foot surgery is often chosen as the last available option for conditions that have otherwise been unsuccessfully treated. Surgery may be necessary for several reasons, including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems, reconstruction due to injury, and congenital malformations (e.g. club foot or flat feet). Regardless of one’s age, foot surgery may be the only successful option for treatment for certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has. For the removal of a bunion growth, a bunionectomy is necessary. If the bones in the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For pain or nerve issues, a patient may require surgery in which the tissues surrounding the painful nerve are removed. Initially, less invasive treatments are generally attempted; surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes with certain benefits. The associated pain experienced in relation to the particular condition is often relieved with surgery, allowing patients to quickly resume daily activities. The greatest benefit, however, is that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. In the field of foot surgery, endoscopic surgery is just one of the many advanced forms of surgery. As technology vastly improves so too will the various techniques in foot surgery, which already require smaller and smaller incisions with the use of better and more efficient tools. Thanks to such innovations, surgery is no longer as invasive as it was in the past, allowing for faster and easier recoveries.
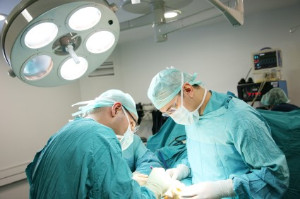
Ankle arthroscopy represents a minimally invasive surgical procedure used to diagnose and treat a variety of ankle joint problems. Through small incisions, a podiatrist inserts a tiny camera, called an arthroscope, into the ankle joint, allowing for a detailed examination of its structures. This procedure offers several advantages over traditional open surgery, including smaller incisions, reduced postoperative pain, and quicker recovery times. Ankle arthroscopy can be used to address a range of conditions, such as ankle impingement, ligament tears, cartilage damage, and loose bodies within the joint. During the procedure, specialized instruments may be utilized to repair or remove damaged tissue, restore joint stability, and alleviate symptoms. By providing direct visualization of the ankle joint, arthroscopy enables precise diagnosis and targeted treatment, ultimately facilitating improved outcomes for patients experiencing ankle-related issues. As a minimally invasive approach, ankle arthroscopy continues to evolve, offering patients a less disruptive option for resolving ankle joint problems. If you have chronic ankle pain, it is suggested that you are under the care of a podiatrist who can determine if ankle arthroscopy is right for you.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact one of our podiatrists of Cascade Foot & Ankle. Our doctors will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.