Yakima
(509) 225-3668
Ellensburg
(509) 925-4633
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot or ankle area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person's joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
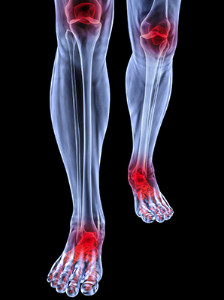 The condition known as rheumatoid arthritis is a painful ailment that typically affects the muscles and joints. When this occurs in the feet, the toenails may become affected in addition to the patient possibly experiencing pain and stiffness. The discomfort is generally felt in the smaller joints in the feet, and this can possibly lead to the formation of corns and bunions. In severe cases, the toes may curl and hammertoe may develop as a result of this. This particular form of arthritis occurs when the body’s immune system is compromised. The ability to fight infection is diminished, and this may cause pain and swelling to gradually develop. If you are afflicted with rheumatoid arthritis in the joints of the feet, it’s strongly suggested that you consult with a podiatrist, so correct treatment can commence.
The condition known as rheumatoid arthritis is a painful ailment that typically affects the muscles and joints. When this occurs in the feet, the toenails may become affected in addition to the patient possibly experiencing pain and stiffness. The discomfort is generally felt in the smaller joints in the feet, and this can possibly lead to the formation of corns and bunions. In severe cases, the toes may curl and hammertoe may develop as a result of this. This particular form of arthritis occurs when the body’s immune system is compromised. The ability to fight infection is diminished, and this may cause pain and swelling to gradually develop. If you are afflicted with rheumatoid arthritis in the joints of the feet, it’s strongly suggested that you consult with a podiatrist, so correct treatment can commence.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact one of our podiatrists of Cascade Foot & Ankle. Our doctors will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
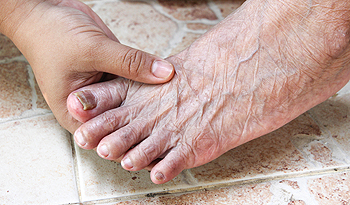 A condition that is referred to as onychomycosis is commonly known as a fungal infection of the toenails. It is common among people who have sweaty feet or enjoy spending time swimming. It may occur as a result of the small fungi seeping through tiny cuts in the skin, or possibly lodging between the nail and the nail bed. It may be common to find this type of infection in the toenails because of the warm environment the shoes and socks provide. There are several symptoms associated with this condition, including having a yellow, white or brown appearance, the nail becoming brittle and breaking easily, or the nail becomes uncomfortable. Despite the unsightly appearance, they typically do not pose a health threat unless the patient is diabetic. Research has shown there may be preventative measures that can be taken, including washing and drying the feet, especially between the toes, trimming the nails properly and frequently, and avoiding wearing other people’s shoes. If you feel you have a toenail fungus, it’s suggested to speak with a podiatrist as quickly as possible for a correct diagnosis and to learn about treatment options.
A condition that is referred to as onychomycosis is commonly known as a fungal infection of the toenails. It is common among people who have sweaty feet or enjoy spending time swimming. It may occur as a result of the small fungi seeping through tiny cuts in the skin, or possibly lodging between the nail and the nail bed. It may be common to find this type of infection in the toenails because of the warm environment the shoes and socks provide. There are several symptoms associated with this condition, including having a yellow, white or brown appearance, the nail becoming brittle and breaking easily, or the nail becomes uncomfortable. Despite the unsightly appearance, they typically do not pose a health threat unless the patient is diabetic. Research has shown there may be preventative measures that can be taken, including washing and drying the feet, especially between the toes, trimming the nails properly and frequently, and avoiding wearing other people’s shoes. If you feel you have a toenail fungus, it’s suggested to speak with a podiatrist as quickly as possible for a correct diagnosis and to learn about treatment options.
For more information about treatment, contact one of our podiatrists of Cascade Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
 Patients who are diabetic often experience conditions involving the feet. These may include corns, blisters, and foot ulcers, which may typically be a result of elevated blood sugar levels. Many patients experience a tingling sensation and this may prevent cuts, sores, and bruises from being noticed. There are several preventative measures to ensure the feet can feel good. These generally include inspecting the feet daily for any type of cuts or wounds, maintaining dry feet to reduce the possibility of infection, and always wearing shoes or having your feet covered while inside or outside. Additionally, if smoking is part of the patients daily routine, research has shown it is advised to quit, and this may improve circulation in the feet. If you are diabetic, it’s suggested to have your feet checked regularly by a podiatrist who will be able to properly treat any foot conditions related to diabetes.
Patients who are diabetic often experience conditions involving the feet. These may include corns, blisters, and foot ulcers, which may typically be a result of elevated blood sugar levels. Many patients experience a tingling sensation and this may prevent cuts, sores, and bruises from being noticed. There are several preventative measures to ensure the feet can feel good. These generally include inspecting the feet daily for any type of cuts or wounds, maintaining dry feet to reduce the possibility of infection, and always wearing shoes or having your feet covered while inside or outside. Additionally, if smoking is part of the patients daily routine, research has shown it is advised to quit, and this may improve circulation in the feet. If you are diabetic, it’s suggested to have your feet checked regularly by a podiatrist who will be able to properly treat any foot conditions related to diabetes.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Cascade Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
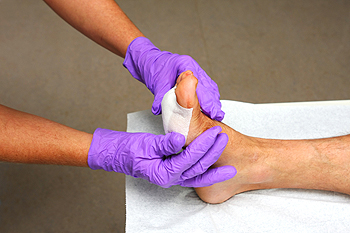 It’s important for most people to check their feet frequently for abnormal conditions, and this is especially true for diabetic patients. If cuts, scrapes and blisters are not noticed, the chances of developing an infection may be amplified because of the body’s inability to heal efficiently. If there are wounds on the feet, recent research has shown the importance of resting frequently, which takes pressure off of the affected area. If you notice cuts on your feet and ankles, it’s suggested to consult with a podiatrist as quickly as possible. At this time a treatment plan can be discussed, which may include what type of wound dressing to use and how often it should be changed. It may be helpful to the patient and may aid in the healing process if the blood sugar levels can be controlled by maintaining a healthy diet and gentle exercise plan.
It’s important for most people to check their feet frequently for abnormal conditions, and this is especially true for diabetic patients. If cuts, scrapes and blisters are not noticed, the chances of developing an infection may be amplified because of the body’s inability to heal efficiently. If there are wounds on the feet, recent research has shown the importance of resting frequently, which takes pressure off of the affected area. If you notice cuts on your feet and ankles, it’s suggested to consult with a podiatrist as quickly as possible. At this time a treatment plan can be discussed, which may include what type of wound dressing to use and how often it should be changed. It may be helpful to the patient and may aid in the healing process if the blood sugar levels can be controlled by maintaining a healthy diet and gentle exercise plan.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with one of our podiatrists from Cascade Foot & Ankle. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Yakima and Ellensburg, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.